.webp)
Get the latest on how to keep your smile healthy and sparkling for the longrun.
Text (404) 816-2230 to Schedule

Looking for Invisalign in Johns Creek? Learn what to look for in a provider, how treatment works, how long it takes, and why patients choose Atlanta Dental Spa.


Looking for the best dentist in Johns Creek GA for veneers? Atlanta Dental Spa specializes in natural-looking, high-tech porcelain smile design. Start your transformation today!


Through patient-first care, luxury experience, and consistent clinical success, Atlanta Dental Spa earns the 2026 Best Dentist in Atlanta from Bulletproof Dental Podcast.


Restore comfort, balance, and confidence with full mouth rehabilitation at Atlanta Dental Spa. Expert planning, complete restorations, and lasting results.

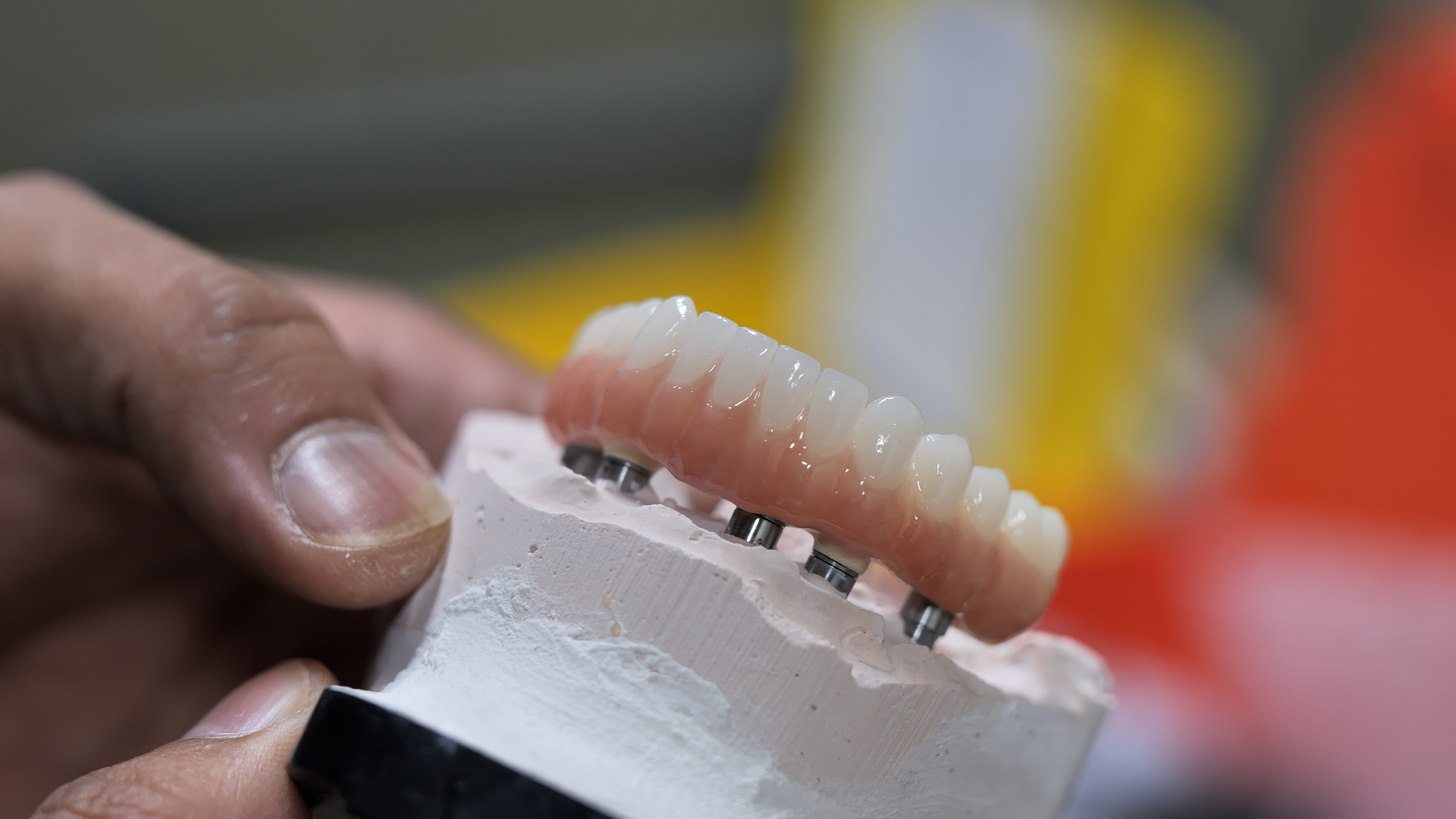
Explore the top teeth restoration options for 2025. From bonding and veneers to implants and bridges. Achieve durable, natural results at Atlanta Dental Spa.


Regain bite strength, clear speech, and lasting comfort with complete dental restorations in Brookhaven, GA. Call (404) 800-0140 or schedule your consultation today.
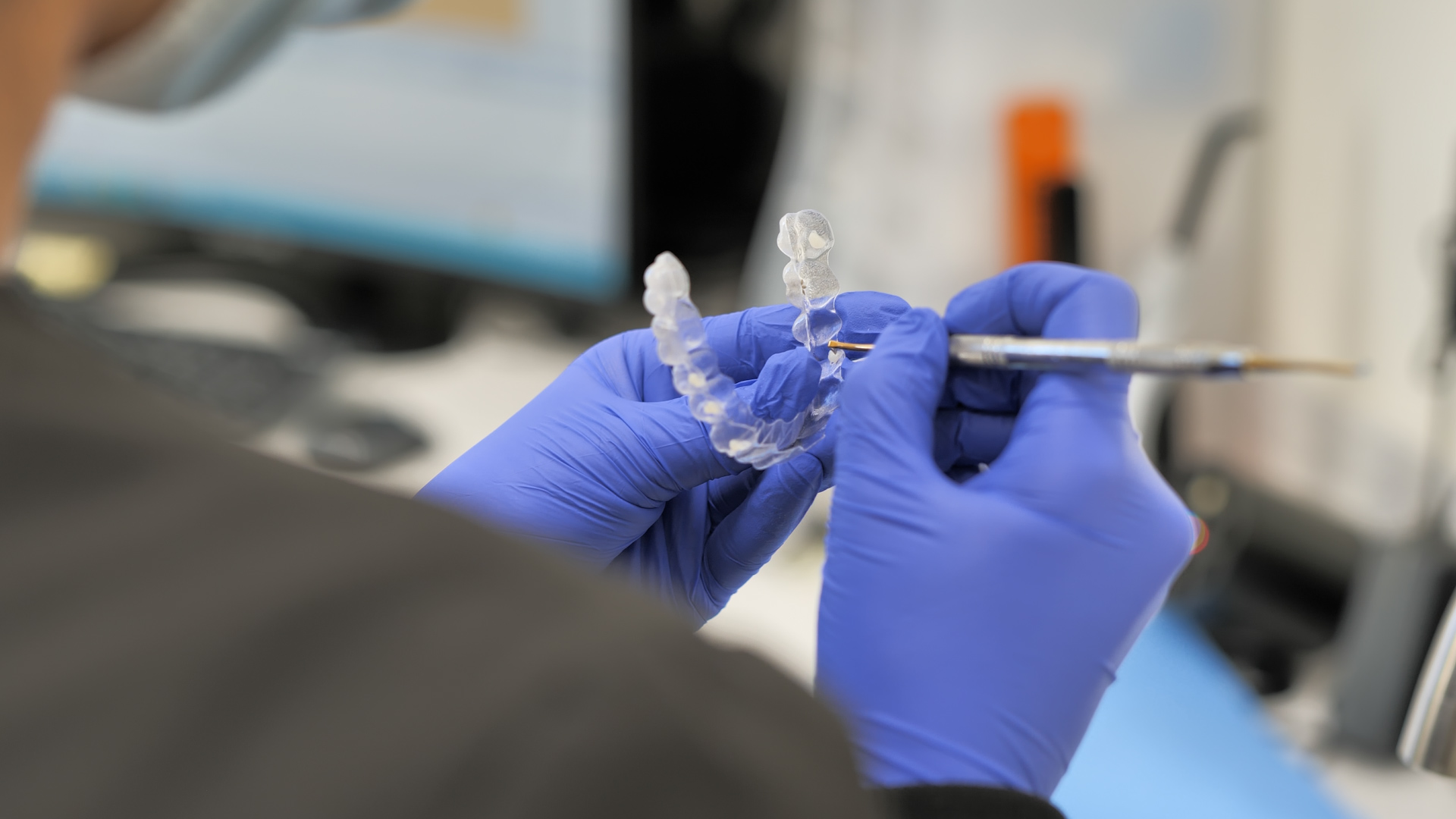

Learn how Invisalign treatment helps adults and teens get a straight smile with comfort and confidence. Enjoy clear aligners, fewer visits, and lasting results.


The difference between Invisalign and braces. Compare costs, comfort, and results to find which treatment gives you the best value for your smile.
.png)
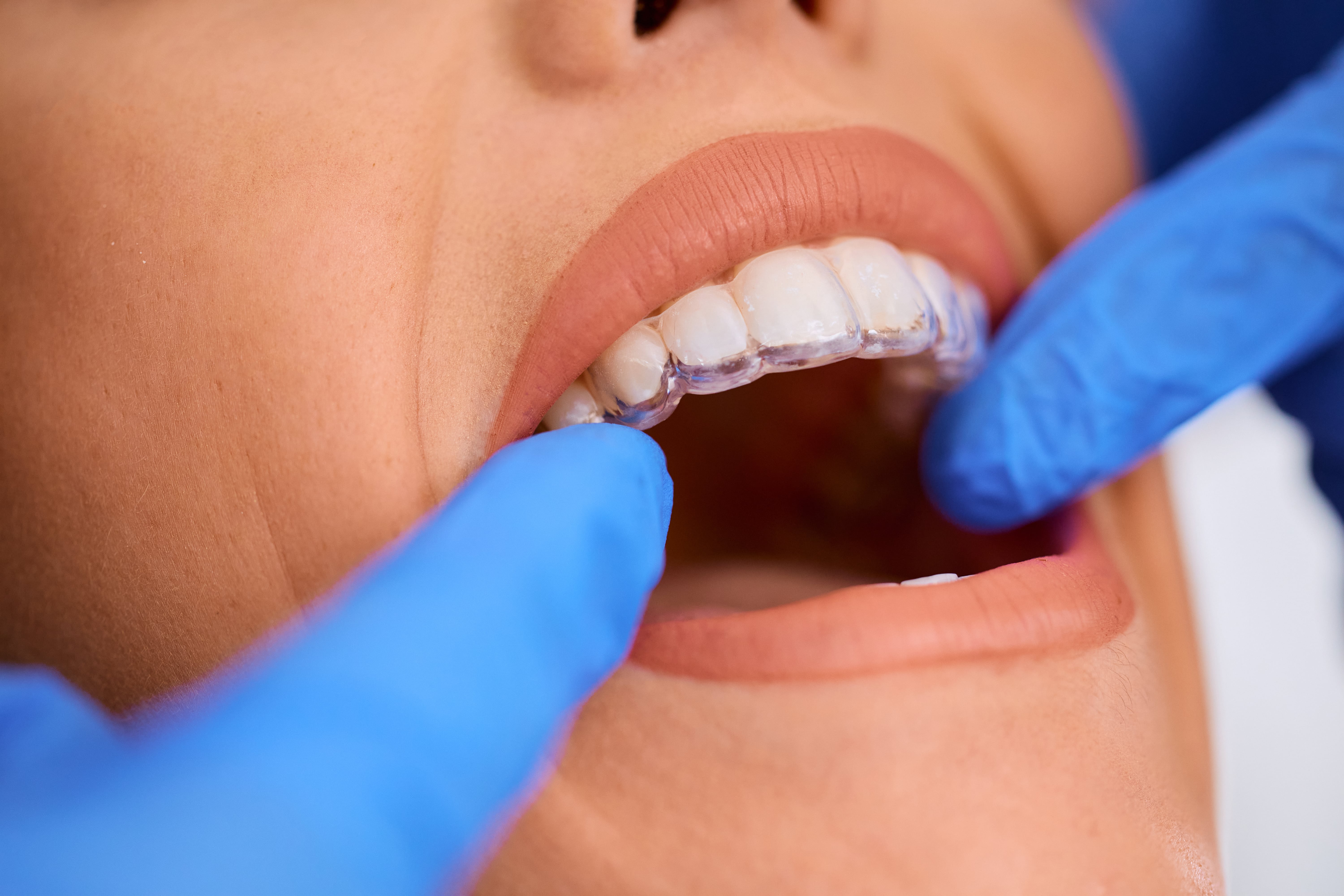
Find out how much Invisalign costs in 2025 and how insurance can help reduce your expenses. Simple, clear info to make your smile treatment affordable.
.webp)
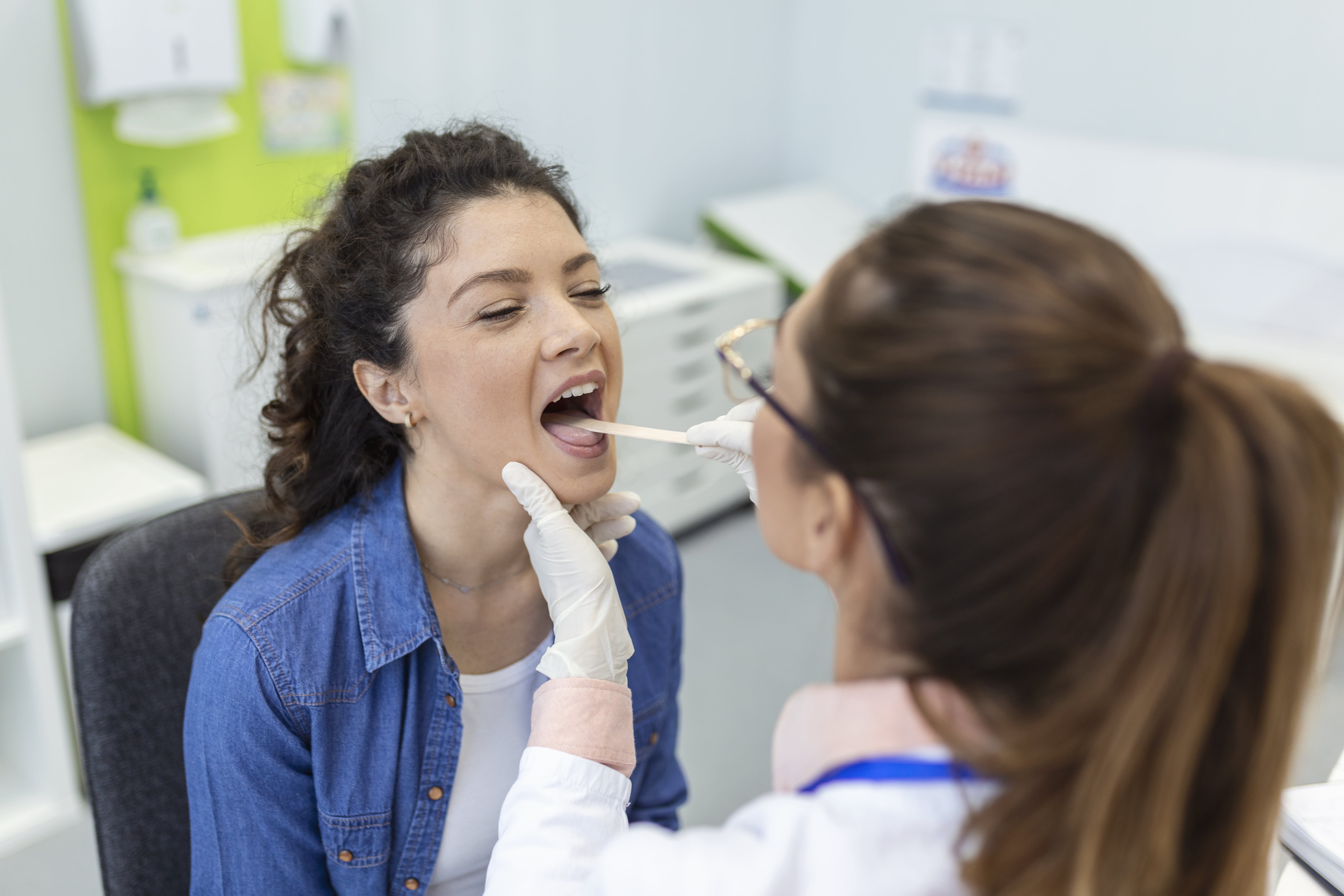
Dental anxiety is a common issue for many patients, frequently leading them to postpone or avoid treatment altogether.
.jpg)
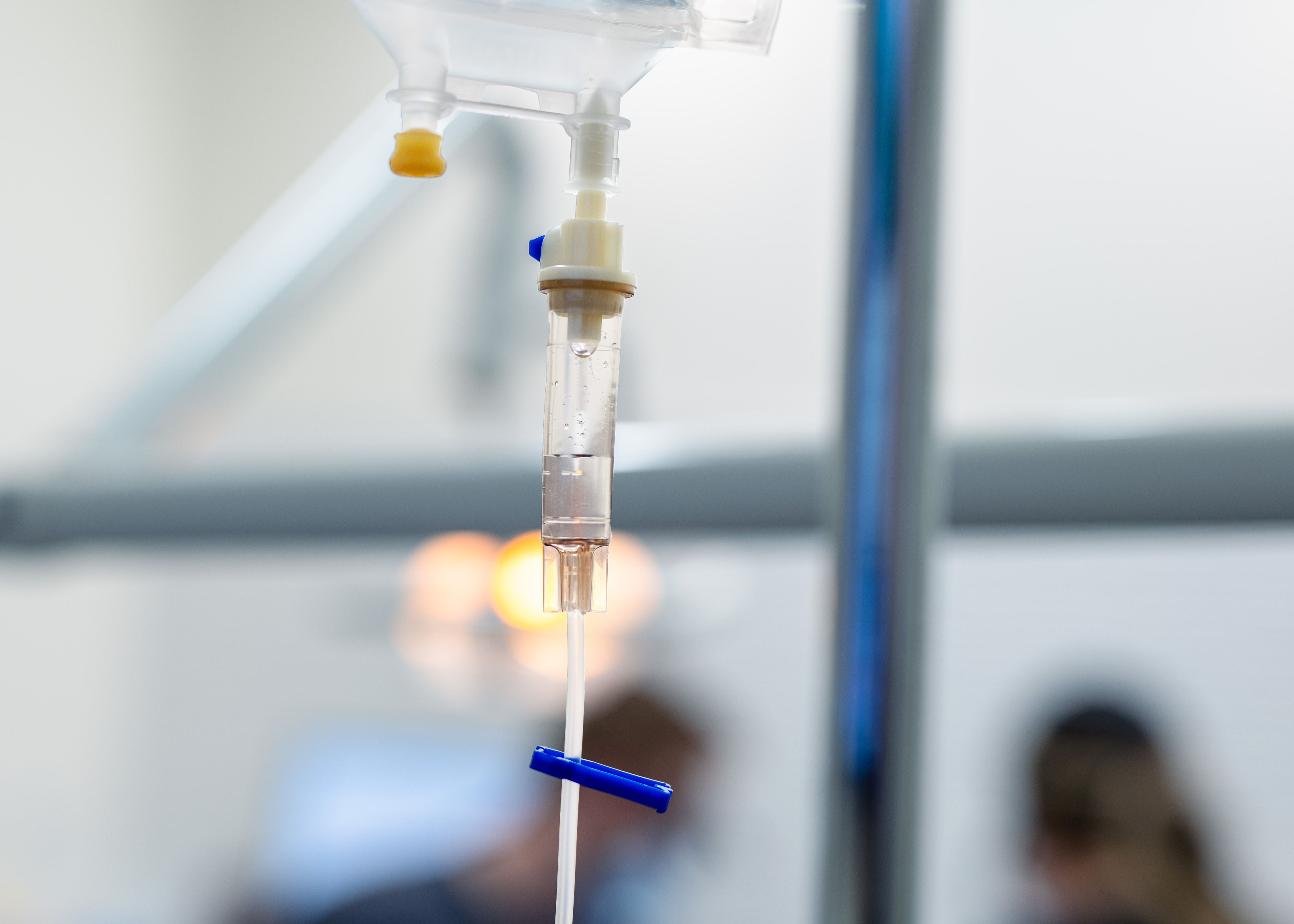
Visiting the dentist is a source of anxiety for many people. It can prevent those with dental anxiety from getting the care they need.

.jpg)
Visiting the dentist may be nerve-wracking for many people, especially those with dental anxiety.
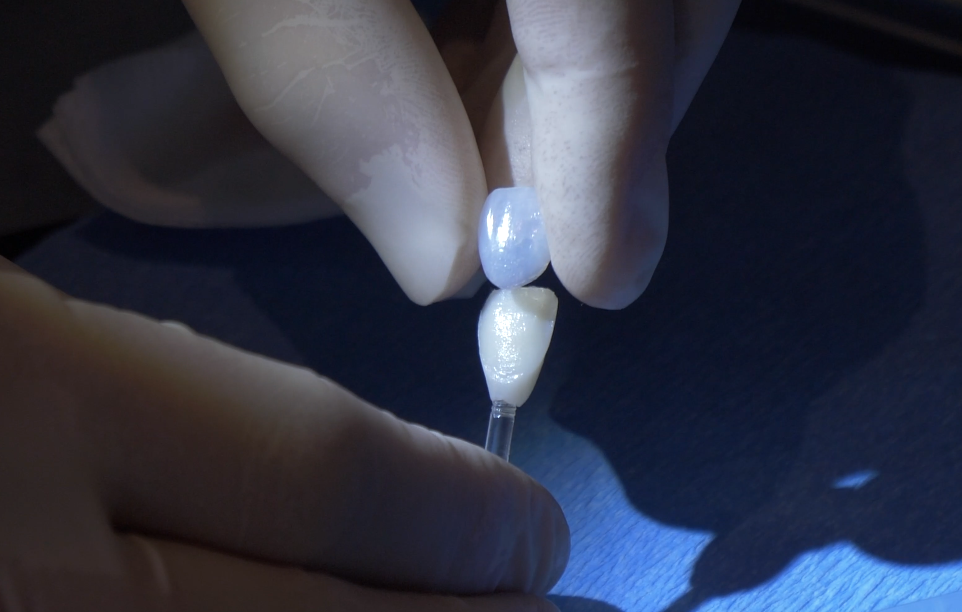

If you are planning to improve your smile in Brookhaven, veneers remain one of the most popular cosmetic dentistry options in 2025.


Achieve the perfect smile with Veneers in Brookhaven GA. Atlanta Dental Spa delivers personalized, lasting porcelain veneer solutions.


If you are looking for veneers in Brookhaven GA, then look no farther than Atlanta Dental Spa. In this article we are going to break down all the information you need to know before getting veneers.
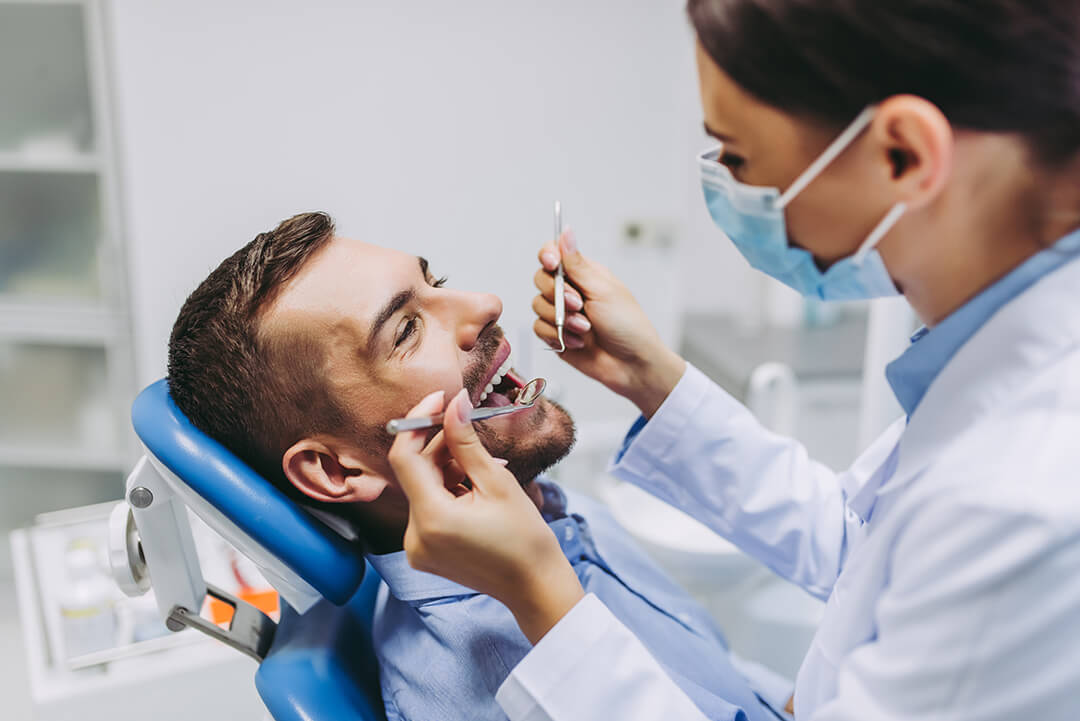

How long does Botox last? Botox results typically last 3–6 months, with duration influenced by age, treatment area, lifestyle, and provider technique.


How long does Invisalign take? Invisalign usually takes 12–18 months, but simple cases may finish in 6–9 months, while complex cases can take up to 24 months.


What are the types of dental fillings? The main types of dental fillings are composite, amalgam, gold, porcelain, and glass ionomer, each offering different strengths, durability, and aesthetics.


Do teeth whitening strips actually work? yes, but only up to a point. Whitening strips can lighten teeth slightly, but the results are often temporary, uneven, and limited compared to professional whitening treatments. Before you invest time and money into at-home strips, it’s worth understanding how they work, their pros and cons, and why professional whitening remains the gold standard for long-lasting results.


What are the 3 types of dental implants? The three types are endosteal implants, subperiosteal implants, and zygomatic implants.


How long do dental implants last? Dental implants can last 25+ years, often a lifetime, while the crown usually needs replacement every 10–15 years.


How long does dentist numbing last? Most dental numbing lasts 1–3 hours, but complex procedures may keep you numb for up to 5 hours.


How much is teeth whitening at dentist? On average, professional teeth whitening costs between $300 and $1,000 per session, depending on the treatment type, location, and dentist’s expertise.


Dentist Who Specializes in Dentures Near Me local denture specialist ensures a comfortable fit, natural look, and ongoing care so you can chew, speak, and smile confidently.


What is general dentistry? General dentistry is primary oral care, including check-ups, cleanings, fillings, and preventive treatments to keep teeth and gums healthy.

No Dental Insurance? Atlanta Dental Spa’s savings plan makes getting care easy. No waiting, no caps, no stress. Just real savings and better health.


Top Rated Dentist in East Cobb and Marietta: Atlanta Dental Spa

Atlanta Dental Spa delivers exceptional, personalized dental care, proudly independently owned and patient-focused since 2004.

Uncover the surprising link between teeth and aging. Learn how to maintain a youthful look with expert dental advice.

Are you experiencing any pain on biting? Are your teeth very sensitive? Do you see any holes in your teeth? Do you have any black or brown spots in your teeth? If any of those apply, chances are you have a cavity.

Dental work overseas may cost less, but is the risk worth it? If you are looking into going out of the country for dental work of any kind, we suggest you reconsider - or at the very least, do your research.

We want to tell you all about one of our latest technologies that has brought Atlanta Dental Spa NEXT LEVEL.

So if you have a gummy smile and you're wondering why, there are a few reasons.

Top Dentists in Atlanta: Your Guide to Exceptional Dental Care!


Discover how AI technology enhances dental care at Atlanta Dental Spa. Precision diagnostics and patient care redefined.


Explore the top 16 reasons why Atlanta Dental Spa is your go-to for exceptional dental care. Elevate your smile and experience the difference today.


Activated Charcoal for Teeth Whitening: Miracle or Myth?Activated charcoal is buzzing in the health and beauty scene, finding its way into a myriad of products from detoxifying smoothies to whitening toothpastes.


Only 4% of Georgia Dentists have IV Sedation permits. Atlanta Dental Spa is proud to have this elite sedation dental service at all 5 locations!


Atlanta Dental Spa has received the unique honor of being voted the "Best Cosmetic Dentist of 2024" by their communities twice. Find out why!


Practitioners of esthetic dentistry are to smile design as Starbucks baristas are to the perfect latte. Point being, you want the most skilled individuals performing this most important of jobs, and the dynamics behind your smile (in addition to your morning coffee) should be left to the professionals! Imagine flashing your pearly whites while the dental team is giving jumping high fives to each other and the Rocky Theme Song resounds through the office!

Explore the reasons and implications of SmileDirectClub's surprising closure. Understand its impact on the industry and your options moving forward.

If you’re searching for a Buckhead dentist who will give you a radiant smile, look no further than Atlanta Dental Spa, a full-service practice that specializes in cosmetic dentistry.

Plan a Vacation to Atlanta for Long-Distance Dental Treatment!

Dentistry is changing in a major way, especially within the last 5 years. Dentisty is becoming far less invasive. For patients, that means less drilling, and better outcomes.

Expertise from Dr. Boulden to find your ideal cosmetic dentist. Transform your smile with top insights for exceptional dental aesthetics.

What comes to mind when you think of cosmetic dentistry? Many of our Atlanta clients are shocked to find how comforting visiting the dentist can actually be!

When some people think of cosmetic dentistry, they think about getting porcelain veneers and looking like they’ve got a million dollar smile (kind of like a movie star). Conversely, when most people think about getting dentures, they think of false-looking teeth that don’t stay in the mouth very well.

If your smile isn’t what you want it to be, then high quality porcelain veneers or Lumineers could be the perfect option for you. However, many people do not consider these options, because they assume financing is not available for porcelain veneers. If you have always wanted veneers to create that brilliant, priceless smile (but didn’t think you could afford them) we have the solution for you!

High-quality porcelain veneers enhance your smile for many years to come, making them one of the best investments in cosmetic dentistry. Cheap veneers, on the other hand, may look fake and will likely need to be repaired or replaced within a few years.


Looking for dental implants in Atlanta? Get the best prices and quality care for a confident, beautiful smile. Learn more now!

Expert advice from Atlanta Dental Spa on selecting quality veneers. Elevate your smile with our detailed guide on what to look for in premium veneers.

There is a lot of disinformation out there on the internet. Dr. Hamilton is here to bust a few DENTAL MYTHS!

Are your teeth sensitive? Do you struggle with whitening because you find it painful? We have answers for you!

I'm Dr. King. For whatever reason, this past weekend I had 5 people ask me the same question, "Do you floss first or do you brush first?" The team here at Johns Creek has mixed opinions!

Are you embarrassed by your smile? Are your teeth breaking or falling apart? Are you in a denture that you currently hate or you just can't stand how it fits? If any of those questions apply to you, we have a great solution for any and all of those issues.

Hi! I am Charissa Wood, I'm one of the hygienists here at Atlanta Dental Spa. I want to talk about some really cool, new technology that we have just embraced at our Johns Creek location - and actually at all 4 of our locations! It's called the iTero scanner.

Here at Atlanta Dental Spa, we are a JUDGEMENT FREE ZONE! We know finding your dental home is scary, especially when you are in pain or have been struggling with your oral health, but we are here to help.

How do I whiten my teeth? We here at Atlanta Dental Spa can whiten your teeth in 3 different ways.

So you want your dream smile, but you don't want the hassle of going to the dentist to see what it would look like?

One of the questions I commonly get when someone is interested in a smile redesign or getting veneers is, "How do we pick the shade?" We actually use a shade guide.

Hey guys! We're here with Sara today. She has been having a lot of TMJ pain and a lot of clenching and grinding. Today we're going to see if we can correct those problems!

There are a lot of frequently asked questions that we get. A lot of time we get questions about whitening, clenching and grinding - for a lot of patients it has been a long time since they've been in, so there's usually a lot of topics that we discuss in the first visit.

One of the most common Invisalign questions I get is, "Do they hurt?" Maybe a very mild sensation of pressure - I've never had a patient complain about sensitivity from the clear aligners. It's a much more gradual impact of movement compared to braces.

We get questions about dry socket all the time. What is dry socket? A lot of people know that buzz word because it's not a fun thing when it happens and it's a fairly common thing in lower wisdom tooth extractions especially.

TMJ symptoms can include headaches, jaw pain, pain when you bite down, pain when you open, sometimes you can even experience clicking in your jaw joint. We have a variety of treatment options for these symptoms.

Flossing is really important because it disrupts bacteria both between the teeth and below the gum line, if you're doing it right. So that's what we want to talk about.